On Thursday, 11th September 2025, Dr Babajide Ogunlana attended the monthly Diabetes Association of Nigeria (DAN) support group session at Gbagada General Hospital, Lagos 🇳🇬. The DAN support group provides education, screenings, and psychosocial support to people living with diabetes, with the aim of reducing complications and helping individuals manage their condition more effectively.
During the session, diabetic foot screenings were conducted — some by Dr Ogunlana himself and others by trained DAN members who have been empowered over the years to carry out diabetes foot checks.
One particularly memorable encounter involved a gentleman who had recently undergone a right leg amputation due to diabetic foot complications. He was observed to be barefoot on his remaining left foot. Upon questioning, the patient explained that he lacked sensation in that foot and that his shoe frequently fell off when using crutches.
Dr Ogunlana expressed deep concern and took the opportunity to educate the patient extensively about the risks associated with walking barefoot — especially in individuals with diabetes. The patient was identified as high-risk for further injury, potentially leading to ulcers or another amputation. To support him, a post-operative shoe was donated, and clear guidance was provided on the importance of wearing protective footwear.
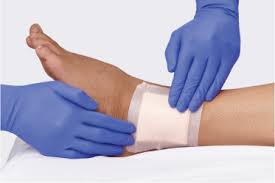
Another notable case involved a patient with a slow-healing wound on the lateral side of the left ankle. Wound care was administered to prevent infection, and a broader discussion was held on associated conditions such as athlete’s foot, fungal toenails, dry skin, skin fissures, peripheral neuropathy, and circulatory issues — all common complications in diabetes care. The patient received wound dressing supplies along with personalised care instructions.
The session was described as highly interactive and impactful, with Dr Ogunlana noting the commitment of both DAN facilitators and patients alike. He expressed his appreciation for the ongoing efforts of the DAN Gbagada chapter and looks forward to participating in events surrounding World Diabetes Day on 14th November 2025.
View Photos: