Psoriasis, may be at higher risk for the COVID-19 virus
The authors of a recent study suggest that patients with some dermatologic diseases, such as superficial fungal infections and psoriasis, may be at higher risk for the COVID-19 virus, due to a possible similarity between cutaneous and mucosal immunity.
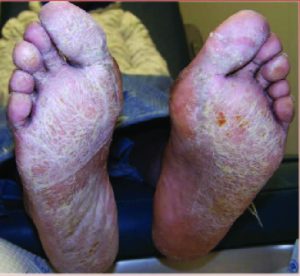
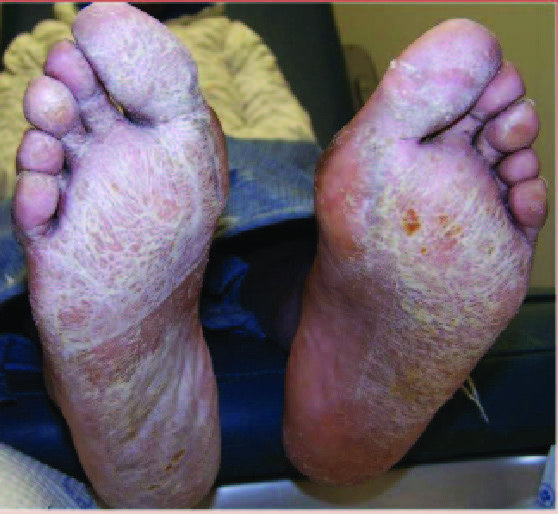
In the study, published by Dermatologic Therapy, researchers assessed dermatological comorbidities of 93 patients with the COVID-19 virus. They found that the most common skin conditions in this patient cohort in the past three years were superficial fungal infections (25.8 percent), seborrheic dermatitis (11.8 percent), actinic keratosis (10.8 percent), psoriasis (6.5 percent) and eczema (6.5 percent).
In addition, 17 of the patients in the study also presented to the dermatology clinic in the last three months. Among this subcohort, the most common dermatological conditions included superficial fungal infections (25 percent), psoriasis (20 percent) and viral skin diseases (15 percent).
Tracey Vlahovic, DPM, FFPM, RCPS (Glasg), says the study authors have made broad assumptions and do not mention other comorbidities or contributing factors. She adds that the study is also problematic since it combines groups receiving topical and systemic/biologic therapy, and suggests that both groups are at risk. Dr. Vlahovic, who is board-certified by the American Board of Foot and Ankle Surgery, recommends monitoring the National Psoriasis Foundation and the International Psoriasis Council websites for guidance.
“The National Psoriasis Foundation recommends those who are on systemic and/or biologic therapy should remain on therapy unless they develop a COVID-19 infection. Patients who have other comorbidities should speak with their physicians regarding staying on their current treatment or changing it,” maintains Dr. Vlahovic, an Associate Professor in the Department of Podiatric Medicine at the Temple University School of Podiatric Medicine.
Joel Morse, DPM agrees that the premise that those with fungal infections or inflammatory skin disease are more likely to contract COVID-19 is suspect.
He wonders if major comorbid conditions such as diabetes could be contributing to an increased risk of developing the COVID-19 virus. Can the virus move through the skin if the stratum corneum is compromised? These are important questions to consider,
says Dr. Morse, a Past President of the American Society for Foot and Ankle Dermatology.
Annette Joyce, DPM concurs that this study has limitations including: a small sample size; lack of specificity as to the location and type of fungal infections involved; and failure to link immunosuppression specifically to these superficial fungal infections.
“Fungal infections of the nails and skin are harder to treat in some patients due to immune system phenotype,” says Dr. Joyce, the Medical Conference Chair for the DERMfoot conference.
Dr. Joyce also notes that organ-specific immune response in the evolving knowledge of antifungal immunity could play a role in future immune-based COVID-19 therapies, but there are still so many unknowns.
Dr. Morse advocates for investigation of other viruses in patients with skin disease, and whether this heightens the risk for infection.
“When someone is in the hospital with COVID-19 life- and limb-threatening issues, we are probably not looking for tinea pedis or scaling on the elbow … but maybe we should,” suggests Dr. Morse, who is board-certified by the American Board of Foot and Ankle Surgery.
Can Adding Plantar Plate Repair To A Metatarsal Osteotomy Yield Better Results For Forefoot Metatarsalgia?
Regardless of the degree of plantar plate injury, adding a plantar plate repair to a shortening second metatarsal osteotomy may improve outcomes, according to a recent study published in the Journal of Foot and Ankle Surgery.
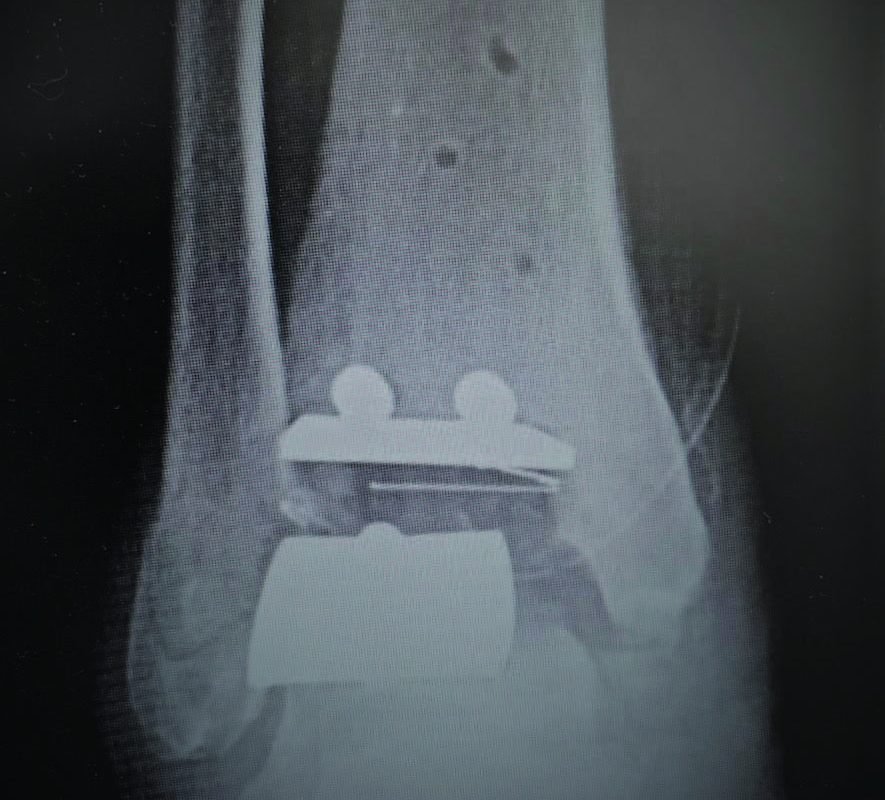
In a prospective study, the authors evaluated 86 adult patients who had second metatarsal Weil osteotomies with and without concomitant plantar plate repair for sub-second metatarsal head pain over a 3.5-year period, and followed them for one year. Patients in the group who had a plantar plate repair with their second metatarsal osteotomy showed better foot-specific quality of life and pain scores at one year despite this group having more severe baseline injuries to the plantar plate. Researchers noted no difference in pre- or postoperative radiographic parabolas, second toe alignment or complication rates between the two groups.
Adam Fleischer, DPM, MPH, FACFAS, the lead author on the study, shares that after successful plantar plate repair from a dorsal approach, he observes patients are less “aware” of their previous foot ailment, which correlates with a higher level of confidence and higher quality of life scores.
Erin Klein, DPM, MS, AACFAS, a co-author of the study, finds in her practice that repairing the plantar plate helps with stability of the MPJ as well as pain.
Dr. Fleischer notes that in his experience, magnetic resonance imaging (MRI) and ultrasound both correlate closely with intraoperative evaluation of the extent of plantar plate injury, which he finds helpful during operative repair.
Dr. Klein agrees. She elaborates that a special MRI protocol with 0.2 to 0.3 mm slices through the metatarsal head/plantar plate region will help the surgeon understand the pathology much better.
“Correcting instability by repairing the plantar plate and then addressing the deforming osseous force (metatarsal length) provides pain relief and improved function postoperatively,” explains Dr. Klein.
Lowell Weil, Jr., DPM, MBA, FACFAS, a co-author of the study, emphasizes the clear necessity to address and correct metatarsal length.
“The plantar plate is a truly important structure that one should repair appropriately when pathology is present,” notes Dr. Weil, CEO of the Weil Foot and Ankle Institute. “Doing this combined procedure yields the highest level results in our research.”
“If patients demonstrate clinical instability of the lesser metatarsophalangeal joint and require a Weil osteotomy, (I recommend) a low threshold for anatomic repair of the plantar plate,” says Dr. Fleischer, who likens it to mechanical instability of the lateral ankle, which benefits from imbrication and advancement of the native tissues.
Are There Identifiable Trends In The Organisms Involved In Osteomyelitis?
What organisms might one expect to see upon bone biopsy in cases of osteomyelitis? A new study in the Journal of Foot and Ankle Surgery takes a closer look at patterns that may help in prescribing effective antibiotics.
Reviewing two random cohorts of 151 patients each in 2005 and 2010, the authors examined demographics, comorbidities, microorganisms found on bone biopsy and culture, location and pre-biopsy antibiotic use. Gram-positive bacteria, specifically methicillin-sensitive Staphyloccus aureus (MSSA), was most common in both groups. However, methicillin-resistant Staphyloccus aureus (MRSA) decreased from a prevalence of 28.3 percent to 10.6 percent from 2005 to 2010. The most common gram-negative bacteria was the Pseudomonas species and patients with peripheral vascular disease exhibited a higher incidence.
Mitzi Williams, DPM, FACFAS, one of the authors on the study, was not surprised by the results as they align with her clinical experience.
Regarding the reduction in MRSA between 2005 and 2010, Dr. Williams personally feels the reason is multifactorial and could include antibiotic stewardship and striving to minimize admissions and returns to the operating room.
Windy Cole, DPM agrees that the findings correlate with her clinical practice. She adds that S. aureus is readily found in the environment as well as the normal skin flora of healthy individuals.
“It is when the bacteria enter into the deep tissues or bloodstream that potentially serious infections can occur,” explains Dr. Cole, the Director of Wound Care Research at Kent State University College of Podiatric Medicine.
MRSA infection reduction could also be attributed to better hygiene, sterilization, and cleaning techniques in the hospital setting and the community, adds Dr. Cole.
Dr. Williams also feels podiatrists approach amputations in a way that prevents future infection.
“We recognize that removal of a central ray will likely result in a transfer lesion and may subsequently become infected,” notes Dr. Williams. “Hence, we do not simply remove what is infected. We perform a functional amputation, which carries lower long-term risks.”
Dr. Cole adds that bone biopsies and deep tissue cultures are the foremost ways to isolate pathogenic bacteria and form the best treatment plan.
Currently, empiric antibiotic use should cover MSSA, says Dr. Williams, a Diplomate of the American Board of Foot and Ankle Surgery. Careful analysis for a history of MRSA, chronic ulcerations or a finding of liquefactive necrosis may lead one to redirect empiric therapy. She adds that one should choose empiric antibiotics based on the most likely organism(s) involved.




 On April 6, 2020, a 13-year-old female presented to the office complaining of severely painful reddish and purple lesions to her toes bilaterally (see top two photos to right). Her symptoms began several weeks
On April 6, 2020, a 13-year-old female presented to the office complaining of severely painful reddish and purple lesions to her toes bilaterally (see top two photos to right). Her symptoms began several weeks  earlier and an ER physician originally treated this as cellulitis with an antibiotic. The condition eventually spread to multiple toes with blisters developing on some of the lesions (see next two photos to right). The pain was so severe the patient
earlier and an ER physician originally treated this as cellulitis with an antibiotic. The condition eventually spread to multiple toes with blisters developing on some of the lesions (see next two photos to right). The pain was so severe the patient type of vasculopathy. The patient denied trauma and did not exhibit any signs or symptoms of infection. The patient had palpable dorsalis pedis and posterior tibial pulses, a sluggish capillary refill time and toes cool to the touch consistent with Raynaud’s disease. The family shared this suspicion as they noted a family history of Raynaud’s disease. At this time, this seemed to be the most likely diagnosis. We dispensed a prescription for nitroglycerin paste for the patient’s pain and symptoms.
type of vasculopathy. The patient denied trauma and did not exhibit any signs or symptoms of infection. The patient had palpable dorsalis pedis and posterior tibial pulses, a sluggish capillary refill time and toes cool to the touch consistent with Raynaud’s disease. The family shared this suspicion as they noted a family history of Raynaud’s disease. At this time, this seemed to be the most likely diagnosis. We dispensed a prescription for nitroglycerin paste for the patient’s pain and symptoms. Ten days later, the patient reported an improvement in her symptoms and clinical presentation, which was confirmed with pictures sent by the patient’s mother (see next two photos to right).
Ten days later, the patient reported an improvement in her symptoms and clinical presentation, which was confirmed with pictures sent by the patient’s mother (see next two photos to right). At this point in time, similar symptoms began to appear in reports of children around the world connected to COVID-19. Further questioning of the patient and her mother confirmed that the patient had a serious flu-like condition the previous month. There were also siblings in the household who had exhibited a fever, sore throat and cough approximately two weeks in duration. These siblings also tested negative for influenza and strep. When the patient began experiencing exhaustion and shortness of breath, she never had testing for influenza due to her siblings’ negative status. She did, however, test negative for mononucleosis. Her pediatrician prescribed an antibiotic and an inhaler. She did not receive a COVID-19 test.
At this point in time, similar symptoms began to appear in reports of children around the world connected to COVID-19. Further questioning of the patient and her mother confirmed that the patient had a serious flu-like condition the previous month. There were also siblings in the household who had exhibited a fever, sore throat and cough approximately two weeks in duration. These siblings also tested negative for influenza and strep. When the patient began experiencing exhaustion and shortness of breath, she never had testing for influenza due to her siblings’ negative status. She did, however, test negative for mononucleosis. Her pediatrician prescribed an antibiotic and an inhaler. She did not receive a COVID-19 test.