By Nicholas A. Campitelli, DPM, FACFAS and Kelly Kubiak DPM
COVID-19, caused by the novel coronavirus named SARS-CoV-2, causes a variety of clinical symptoms with the most common symptoms being a dry cough, fever, myalgia and fatigue.1 Less common symptoms include dyspnea, sputum production and diarrhea. However, as the COVID-19 virus continues to spread across the world, new information about the disease is emerging all the time.
One now hears the term COVID toes being noted when patients who have the COVID-19 virus present with extremity symptoms. These patients may or may not carry an official diagnosis of COVID-19. These patients may present with a digital ischemic appearance of purplish or red lesions on their toe(s) that are often painful.2 However, one could easily confuse the presentation of such symptoms for frostbite, Raynaud’s disease or chilblains. Most reports of such a phenomenon are seen primarily in younger populations with or without other symptoms.3
The exact cause of these symptoms is still unknown. One prominent theory involves a likely underrecognized vascular component to the disease.4 The COVID-19 virus is known to attack cells in the lung via the angiotensin converting enzyme 2 (ACE2) receptor. The ACE2 receptor is not limited to just the lungs. It is also found in other organs including the heart, kidney and intestines. The ACE2 receptor is also found on endothelial cells that line vessels throughout the whole circulatory system, including the very small vessels in the toes.4 Researchers out of the Pathology and Cardiology Departments from University Hospital Zurich, in Zurich, Switzerland speculate that the virus attaching in these small vessels results in the vascular symptoms now known as COVID toes.4
What Recent Case Reports Reveal About COVID Toes
As information on the novel coronavirus continues to evolve, more research on COVID toes may emerge. In a recent report out of China, Zhang and colleagues discussed seven critical patients with the COVID-19 virus, who had an average age of 59 years and clinical symptoms including finger/toe cyanosis, skin bullae and dry gangrene to the digits. These patients also reportedly had prolonged prothrombin time (PT), an elevated D-dimer level and diagnosed disseminated intravascular coagulation (DIC). Five of the seven patients ended up dying from the COVID-19 virus.5
However, most reports on COVID toes come from various news media and seem to be in younger age groups with many of these patients not having any respiratory symptoms.3 A press release from the French National Union of Dermatologists and Venereologists warns of skin manifestations of COVID-19 that the group classifies as acrosyndromes.2 This group defines symptoms as the appearance of pseudo-frostbite, a sudden appearance of persistent and sometimes painful redness, and transient hive lesions on the fingers and/or toes.2
In a recent case study out of Italy from the International Federation of Podiatrists, Mazzotta and Troccoli describe self-healing lesions in children and adolescents, and believe the etiology is vascular in nature.3 Kerri Purdy, MD, FRCPC, president of the Canadian Dermatology Association, also agrees with a vascular origin.6 In a recent interview, Dr. Purdy stated that the presentation is similar to chilblains but she believes the etiology is vascular, not thermal, in nature. She attributes it to small vessel blockages as emerging evidence points to the COVID-19 virus contributing to a hypercoagulable state.6
Physicians in France and Spain also report lower extremity symptoms in various younger populations.2,3 As the aforementioned report out of China shows, COVID toe is not limited to the young but may possibly be the only symptom present in a patient with the COVID-19 virus.5
Our Experience With A Possible Presentation Of COVID-Related Pedal Symptoms
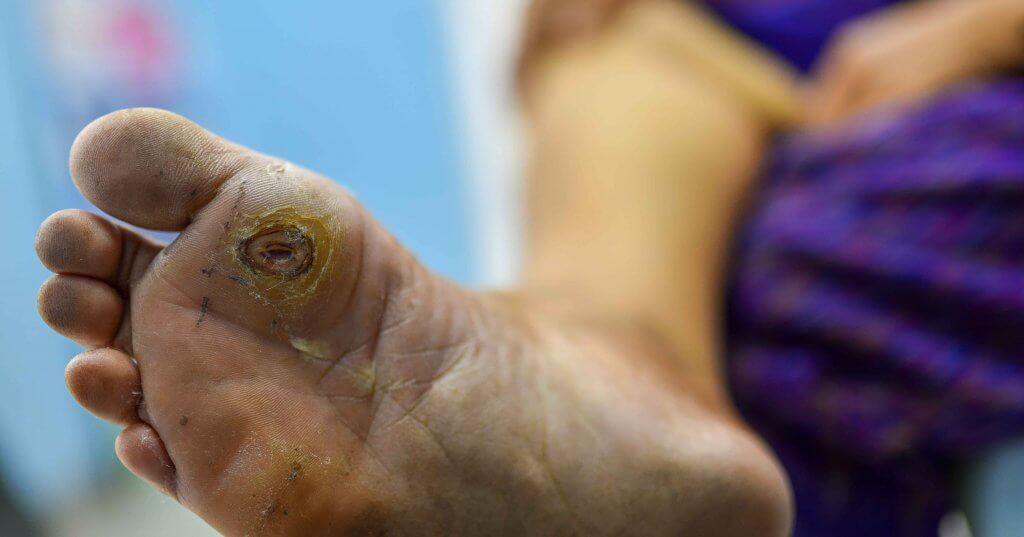
 On April 6, 2020, a 13-year-old female presented to the office complaining of severely painful reddish and purple lesions to her toes bilaterally (see top two photos to right). Her symptoms began several weeks
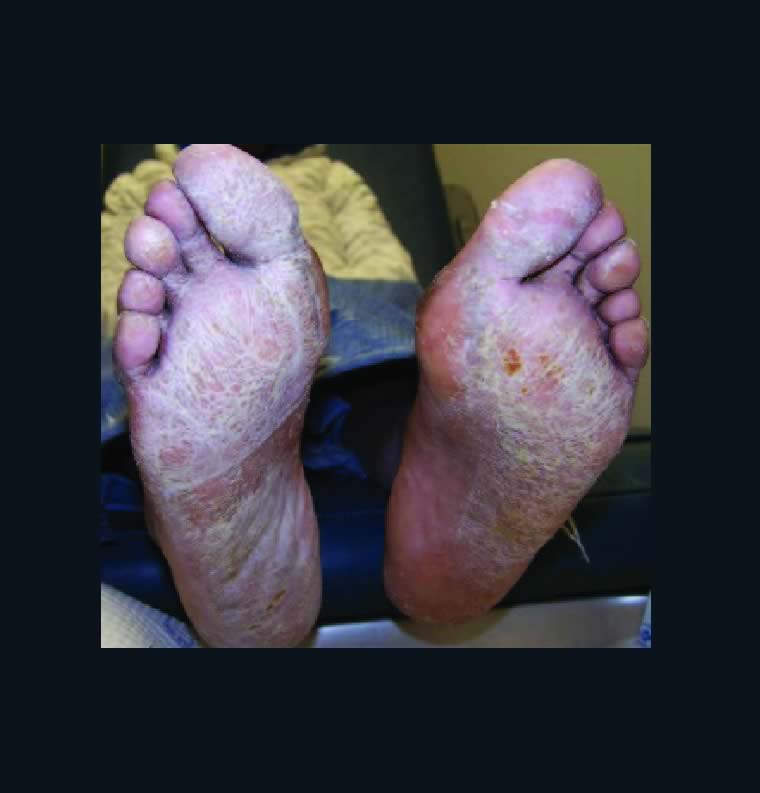
On April 6, 2020, a 13-year-old female presented to the office complaining of severely painful reddish and purple lesions to her toes bilaterally (see top two photos to right). Her symptoms began several weeks  earlier and an ER physician originally treated this as cellulitis with an antibiotic. The condition eventually spread to multiple toes with blisters developing on some of the lesions (see next two photos to right). The pain was so severe the patient
earlier and an ER physician originally treated this as cellulitis with an antibiotic. The condition eventually spread to multiple toes with blisters developing on some of the lesions (see next two photos to right). The pain was so severe the patient could not tolerate shoes.
The initial presentation was consistent with Raynaud’s disease as it was almost certainly some  type of vasculopathy. The patient denied trauma and did not exhibit any signs or symptoms of infection. The patient had palpable dorsalis pedis and posterior tibial pulses, a sluggish capillary refill time and toes cool to the touch consistent with Raynaud’s disease. The family shared this suspicion as they noted a family history of Raynaud’s disease. At this time, this seemed to be the most likely diagnosis. We dispensed a prescription for nitroglycerin paste for the patient’s pain and symptoms.
type of vasculopathy. The patient denied trauma and did not exhibit any signs or symptoms of infection. The patient had palpable dorsalis pedis and posterior tibial pulses, a sluggish capillary refill time and toes cool to the touch consistent with Raynaud’s disease. The family shared this suspicion as they noted a family history of Raynaud’s disease. At this time, this seemed to be the most likely diagnosis. We dispensed a prescription for nitroglycerin paste for the patient’s pain and symptoms.
 Ten days later, the patient reported an improvement in her symptoms and clinical presentation, which was confirmed with pictures sent by the patient’s mother (see next two photos to right).
Ten days later, the patient reported an improvement in her symptoms and clinical presentation, which was confirmed with pictures sent by the patient’s mother (see next two photos to right).
 At this point in time, similar symptoms began to appear in reports of children around the world connected to COVID-19. Further questioning of the patient and her mother confirmed that the patient had a serious flu-like condition the previous month. There were also siblings in the household who had exhibited a fever, sore throat and cough approximately two weeks in duration. These siblings also tested negative for influenza and strep. When the patient began experiencing exhaustion and shortness of breath, she never had testing for influenza due to her siblings’ negative status. She did, however, test negative for mononucleosis. Her pediatrician prescribed an antibiotic and an inhaler. She did not receive a COVID-19 test.
At this point in time, similar symptoms began to appear in reports of children around the world connected to COVID-19. Further questioning of the patient and her mother confirmed that the patient had a serious flu-like condition the previous month. There were also siblings in the household who had exhibited a fever, sore throat and cough approximately two weeks in duration. These siblings also tested negative for influenza and strep. When the patient began experiencing exhaustion and shortness of breath, she never had testing for influenza due to her siblings’ negative status. She did, however, test negative for mononucleosis. Her pediatrician prescribed an antibiotic and an inhaler. She did not receive a COVID-19 test.
Anecdotally, we learned through social media of a 13-year-old male from the same school of the first patient who exhibited similar symptoms and painful complaints about his toes. His symptoms had a six-week duration and consisted of erythema and pain to his toes (see bottom two images to right). The erythema eventually progressed to purpuric-appearing lesions on all of the toes very similar in nature to the previous patient. His
pediatrician prescribed oral steroids three weeks after the initial presentation of symptoms and this treatment eventually allowed the patient to tolerate shoe gear. This patient displayed no clinical symptoms of the COVID-19 virus and had no other pertinent findings such as fever or dermatological lesions elsewhere. Accordingly, the patient was not tested for COVID-19 at that time.
In Conclusion
The aforementioned cases provide anecdotal evidence of two patients in the same geographic area who presented with symptoms that are possibly consistent with COVID toes albeit without a confirmed diagnosis of the COVID-19 virus. Both patients were in their early teens and early reports have suggested that COVID toes appear to be most prevalent in this age group.3 Both patients described color changes and a painful presentation with four to six weeks of symptoms before noting improvement. Only one of the patients exhibited crusted lesions as noted in an aforementioned report out of France.2 One patient had other symptoms suggestive of the COVID-19 virus and the other patient did not. This is consistent with similar findings in another recent report out of Spain that noted COVID toe in both symptomatic and asymptomatic patients.7 While these authors recommended topical corticosteroid treatment for patients with these lesions, other cautions exist regarding the use of systemic steroids in patients with the COVID-10 virus so practitioners should exercise caution in this population.7,8
For the presented patients above, improvement occurred with nitroglycerin paste and topical steroids respectively. It may be prudent to also suggest that similar patients exercise caution and self-quarantine due to the possible association with the COVID-19 virus.
At the present time, there is limited, if any, true scientific literature to guide clinical decision making in the diagnosis of these questionable COVID toes. This presents difficulty in presenting a possible diagnosis yet to be proven scientifically or backed with peer-reviewed literature. With that said, there is evidence to suggest that the two aforementioned patients who presented with pain, red-to-blue colored lesions and vasculitis to their toes could possibly have had COVID toes. The symptom timeline along with the presence of the virus in the United States supports this. Certainly, more research is necessary to specifically correlate known COVID-19 status and COVID toe presentation before we can confirm the true etiology and association of COVID toes.
Dr. Campitelli is the Director of the Podiatric Residency Program at the Western Reserve Hospital in Cuyahoga Falls, Ohio. He is an Adjunct Clinical Professor at the Kent State University School of Podiatric Medicine
Dr. Kubiak is a third-year podiatric surgery resident at the Western Reserve Hospital in Cuyahoga Falls, Ohio.
References
- Huang C, Wang Y, Li X, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet. 2020;395(10223):497-506.
- La Revue du Praticien. Covid revealing acrosyndromes. Available at: https://drogunlana.com/2020/04/30/the-benifits-of-middle-age-fitness/ . Accessed April 27, 2020.
- Mazzotta F, Troccoli T. Acute acro-ischemia in the child at the time of COVID-19. International Federation of Podiatrists. Available at: https://www.fip-ifp.org/wp-content/uploads/2020/04/acroischemia-ENG.pdf. Accessed April 27, 2020.
- Varga Z, Flammer AJ, Steiger P, et al. Endothelial cell infection and endotheliitis in COVID-19. Lancet. 2020. Available at: https://doi.org/10.1016/S0140-6736(20)30937-5. Accessed April 27, 2020.
- Zhang Y, Cao W, Xiao M, et al. Clinical and coagulation characteristics of 7 patients with critical COVID-2019 pneumonia and acro-ischemia. Chinese J Hematol. 2020;41(0):E006.
- Young L. ‘COVID toes’ could be another symptom of coronavirus infection: experts. Global News. Available at: https://globalnews.ca/news/6848644/covid-toes-skin-rash-coronavirus-symptom/ . Published April 21, 2020. Accessed April 27, 2020.
- Consejo General de Colegios Oficiales de Podólogos de España: COVID-19 Compatible Case Register. Available at: https://drogunlana.com/2020/04/30/the-benifits-of-middle-age-fitness/ . Accessed April 27, 2020.
- World Health Organization. Clinical management of severe acute respiratory infection when COVID-19 is suspected. Available at: https://www.who.int/publications-detail/clinical-management-of-severe-acute-respiratory-infection-when-novel-coronavirus-(ncov)-infection-is-suspected . Accessed April 29, 2020.